Specialists claim to have encouraging evidence that shows that the combination of an annual blood test with an ultrasound, could detect the risk of ovarian cancer in women, reducing in 20 percent the chances of death.
Ovarian cancer is often deadly since the tumors are detected too late, so British researchers conducted a study to determine the effect of early detection by testing on the mortality of this disease.
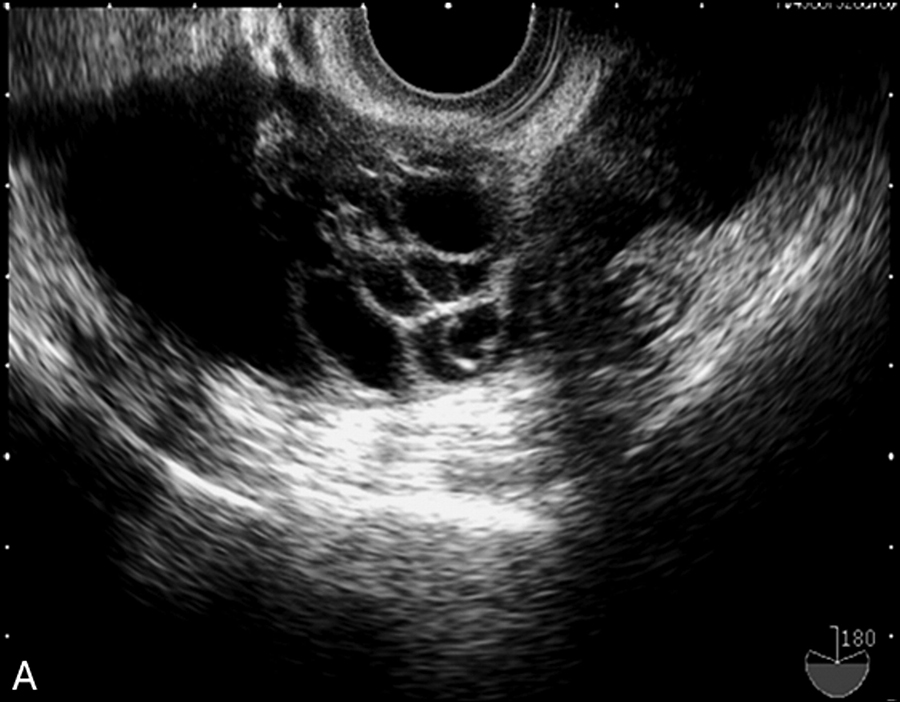
According to the American Cancer Society, this cancer is ranked as the fifth most common cancer among women, causing more deaths than any other in the female reproductive system, as only 40 percent of patients survive five years with it.
Medical specialists studied over 14 years, 200,000 women in the UK, aged 50 to 74. During that time, 1,282 of them were diagnosed with ovarian cancer, and 649 died of the disease. Half the women got no screening. A quarter of the women got an annual ultrasound, and another 50,000 got an annual blood test for CA-125, a tumor marker determined by blood tests and is produced by the ovarian tissue.
During the study, the experts of the gynecological cancer center at University College London, monitored the changes in CA125 levels in the third group, and if they increased, they performed ultrasound to look for evidence of tumors.
Over the time of the study, about 1,200 of the women got ovarian cancer, and they were divided equally among the groups.
Over the whole study period, women who got the blood test and ultrasound screening and who got ovarian cancer, were 15 percent less likely to die than the other women. But after seven years, they were 23 percent less likely to die.
These findings were published in The Lancet journal, stating that when CA125 rises, it is time to act to prevent further problems and have a better chance of survival.
This test was considered as a milestone potential in the early detection of ovarian cancer, although other researchers say it is too early to say that it is fully effective, according to a report published by BBC news.
But it may take some time to become widely available.
“It’s gonna be a debate – do we implement it now because we can save lives potentially, and the risk is there but it’s low?” Dr. David Agus, director of USC Norris Westside Cancer Center, noted that there is also a risk of false positives that could result in some women being put through unnecessary surgery. “Hopefully this will actually mark what we in the cancer world believe in, which really is prevention and early detection. Because that’s going to make the impact,” he said.
Source: CBS News
