Scientists from the University College London have discovered a way to fight antibiotic-resistant superbugs. They have designed new and more effective drugs that can kill superbugs within minutes. They say that drug-resistant bacteria can be killed if the antibiotics push hard enough.
At least 23,000 deaths and 2 million illness occur every year in the United States due to resistant bacteria, according to data published by the Centers for Disease Control and Prevention. Increasing antibiotic resistance threatens society and reduces the advances made in medicine. However, scientists say that vancomycin and oritavancin are super antibiotics that can kill drug-resistant superbug within minutes.
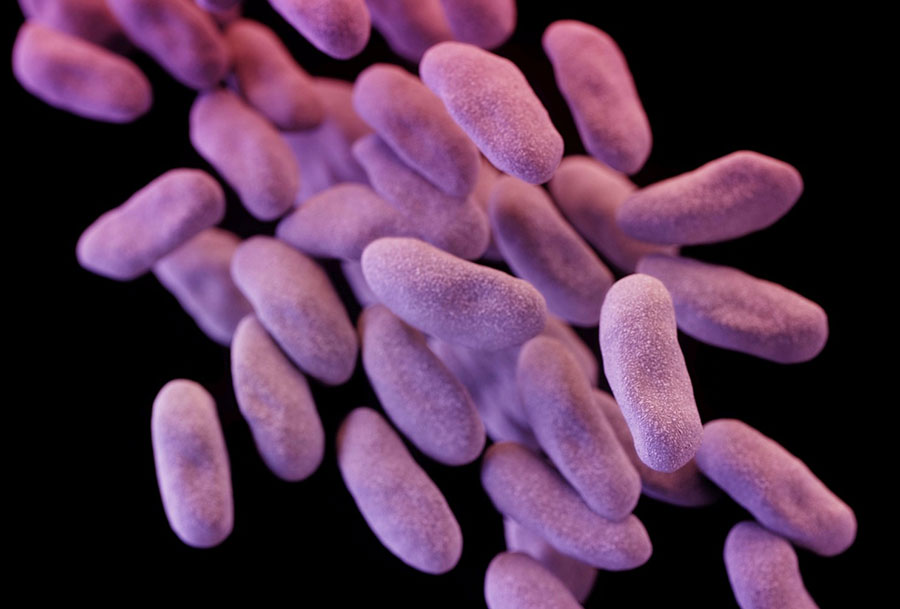
Antibiotics and bacteria are like keys and locks
Some of which were once considered “miracle drugs” have lost the ability to protect people against harmful bacteria. Many bacteria have evolved and mutated to resist the effects of antibiotics. A considerable amount of medical procedures such as surgeries, intense care units, and aggressive cancer chemotherapy require antibiotics to work, but the increasing antibiotic resistance threatens to send society back to the pre-antibiotic era.
Study author Dr. Joseph Ndieyira compared antibiotics and drugs with keys and locks. He said that antibiotics have “keys” that fit into “locks” located on the surface of bacteria. When the keys fit, then they can kill bacteria. When bacteria evolve and develop resistance, then it’s like the locks have been changed. Therefore, the key doesn’t fit. The team discovered that certain antibiotics have the ability to force the locks because they are so strong that they don’t just destroy the locks, they tear doors down, killing the bacteria regardless of how drug-resistant it might be.
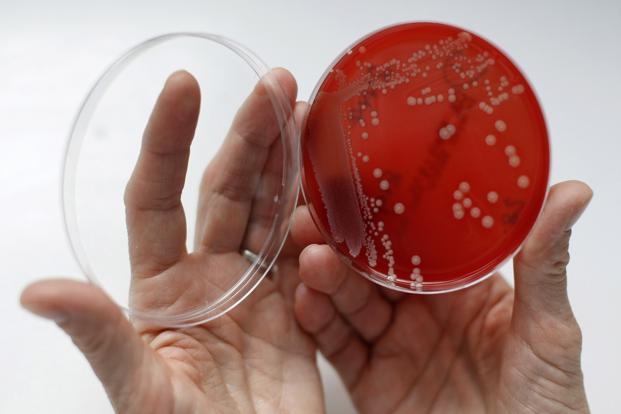
The investigation was published in the Scientific Reports. It was funded by the Engineering and Physical Sciences Research Council, UCL, the NIHR UCLH Biomedical Research Center, and the European Union.
“Incredibly, we found that certain antibiotics can still ‘force’ the lock, allowing them to bind to and kill resistant bacteria because they are able to push hard enough. In fact, some of them were so strong they tore the door off its hinges, killing the bacteria instantly!,” said Dr. Ndieyira.
Antibiotics can kill drug-resistant bacteria if they push hard enough
The scientists measured the performance of four antibiotics on bacteria. They all had similar force on the same type of bacteria, but their force varied when applied to bacteria that had developed resistance to antibiotics. However, scientists said that they could kill any bacteria if they had the right combination of drugs.
The antibiotics that were tested include vancomycin —which is used as the last resource treatment for MRSA (Methicillin-resistant Staphylococcus aureus infections) and other infections given the enormous power it has— and oritavancin, which is a modified version of vancomycin mostly used for complex skin infections. According to the scientists, oritavancin proved to be 11,000 times stronger that vancomycin to fight resistant bacteria.
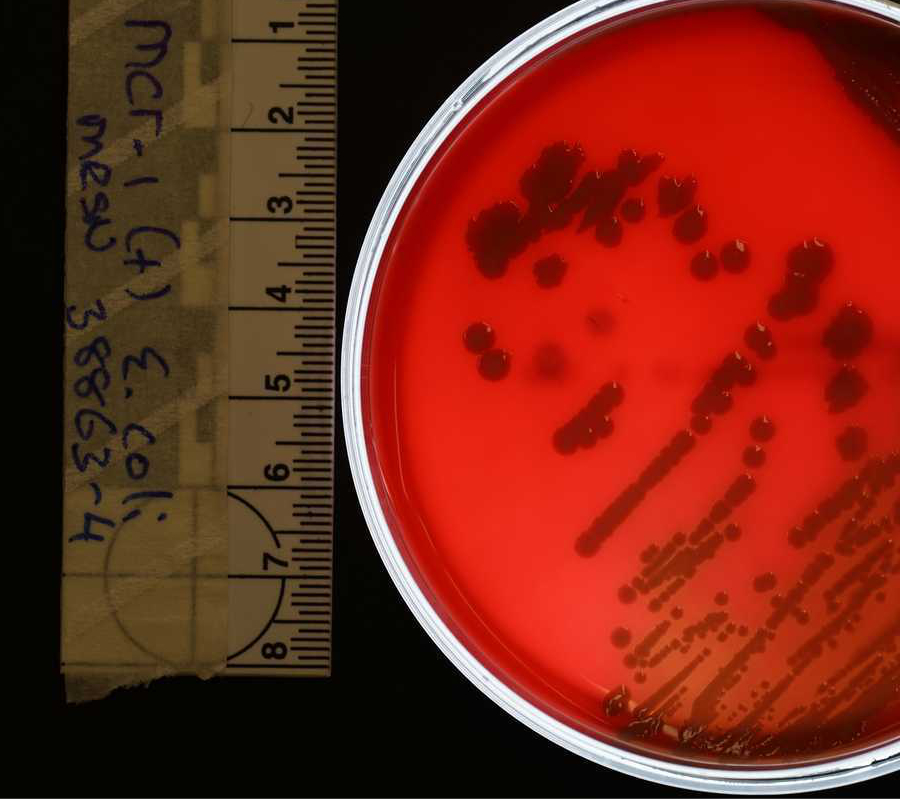
“Even though it has the same ‘key’ as vancomycin, oritavancin was still highly effective at killing resistant bacteria. Until now it wasn’t clear how oritavancin killed bacteria, but our study suggests that the forces it generates can actually tear holes in the bacteria and rip them apart,” said Dr. Ndieyira.
Oritavancin kills bacteria in 15 minutes
Scientists believe that though oritavancin is a modified version of vancomycin, they kill bacteria in a whole different way. Vancomycin works disrupting vital processes in bacteria, stopping their function and making them die slowly. On the other hand, oritavancin molecules stick together forming clusters, and that is what changes everything. When two clusters of oritavancin dig into a bacterial surface, they push apart from each other, tearing the bacteria apart.
“Remarkably, we found that conditions at the bacterial surface actually encourage clustering which makes antibiotics even more effective,” Dr. Ndieyira added.
According to doctor Ndieyira, oritavancin kills bacteria within 15 minutes while vancomycin takes 6 to 24 hours to kill bacteria. The team developed a mathematical model —to describe the actions of antibiotics on the surface of the bacterial cells— that could be key to identify new and more effective drugs. As well, they say the model will be useful to modify the existing antibiotics and make them overcome bacterial resistance.
It is important to remember that people should reduce the unnecessary use of antibiotics to increase its effects. In the U.S. there have been enormous efforts to decrease antibiotic prescriptions per capita as a way to reduce the yearly 23,000 deaths derived from resistance to antibiotics.
Source: The Washington Post
