A group of scientists has invented a new technology that could one day help to heal severe wounds in human organs, Tissue Nanotransfection (TNT). It uses nanotechnology to turn skin cells into other types of cell that can repair damaged tissues.
The research was conducted by scientists at the Ohio State University Wexner Medical Center, and their new study was published online on Monday in the journal Nature Nanotechnology.
The TNT technique has been previously studied in pigs and mice and successfully worked 98 percent of the time. The technology doesn’t require laboratory-based procedures like in stem cell therapy procedures.
Researchers helped mice recover from strokes using TNT nanotechnology
Dr. Chandan Sen, the director of the Ohio State University’s Center for Regenerative Medicine & Cell Based Therapies and co-author of the new study, said that with this technology, they can turn skin cells into cells of any organ with “just one touch.” He noted the process is non-invasive and only takes less than a second.
Sen co-led the study with L. James Lee, a professor of chemical and biomolecular engineering at the university’s College in Engineering. They also worked alongside the Nanoscale Science and Engineering Center of the University.
The researchers used mice and pigs in their experiments. They were able to reprogram skin cells to become vascular cells in injured legs that lacked blood flow. Within one week of using the technique, active blood vessels appeared on the injured leg, and in the second week, the leg was saved, according to the researchers.
In laboratory tests, the scientists also found the technique can also transform body cells into nerve cells to be injected into mice with brain injuries, helping them recover from a stroke.
“This process only takes less than a second and is non-invasive, and then you’re off,” said Sen, according to a statement. “The chip does not stay with you and the reprogramming of the cell starts. Our technology keeps the cells in the body under immune surveillance, so immune suppression is not necessary.”
Researchers to test TNT technology in humans next year
Using the new nanochip technology, compromised or injured organs can be completely replaced, according to Sen. He noted that skin “is a fertile land” where they can grow the elements of any compromised organ.
The new technology has two components: a nanotechnology-based chip designed to carry cargo to adult cells in the live body, and a design of specific biological cargo for cell conversion. Daniel Gallego-Perez, an assistant professor of biomedical engineering and general surgery and first author of the study, explained that the cargo, when delivered using the nanochip, converts an adult cell from one type to another.
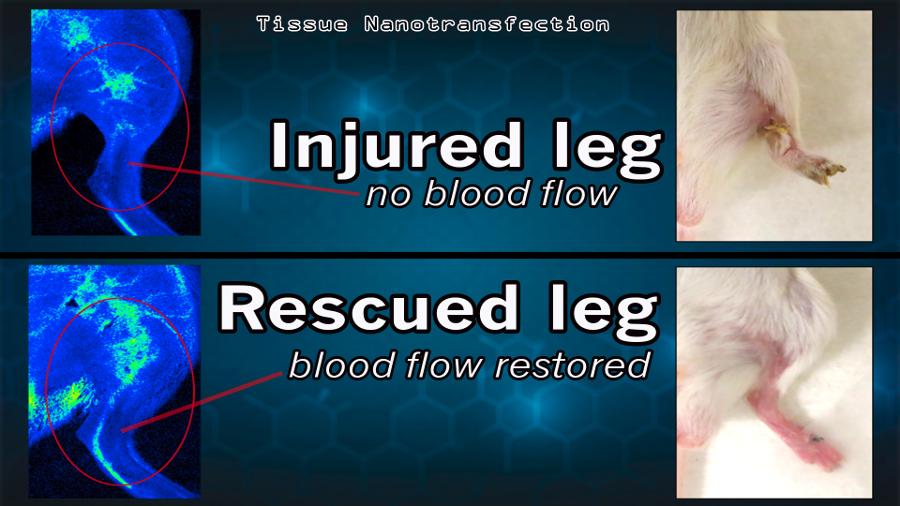
The researchers noted the TNT technology does not require any laboratory-based procedures and can be implemented at the point of care. The cargo is delivered by zapping the chip with a small electrical charge that’s barely felt by the person carrying it.
“The concept is very simple,” said Lee. “As a matter of fact, we were even surprised how it worked so well. In my lab, we have ongoing research trying to understand the mechanism and do even better. So this is the beginning, more to come.”
The researchers said they plan to test the TNT technology in humans next year.
‘Nanotechnology will change cancer treatment within next decade’
The research involving nanotechnology is leading to impressive breakthroughs in medicine. A recent study published in the journal Nature Chemistry studied the technique to create functional cell-permeable Nanobodies (antibodies that have single, monomeric domains) that are able of targeted labeling and manipulation of intracellular antigens.
Those findings can help scientists dig further into the use of immunotherapy. Sam Gambhir, a professor and chair of radiology at Stanford University’s School of Medicine, said that nanotechnology would change the path of cancer treatment and diagnosis in the U.S. within the next ten years.
“We can now detect just a few cancer-associated molecules or circulating tumor cells in the body in just a few millimeters of blood or saliva, or map the boundaries of a brain tumor within millimeters to assess its response to therapy or to plan a surgery,” said Gambhir last year, according to International Business Times.
He added that they have specially designed nanoparticles that can send back a massively amplified signal when they bind to colonic cancer cells and noted they are also working on ways to trigger the self-assembly of nanoparticles as they come across a cancer cell. Gambhir also noted the field has advanced “tremendously” in the past 10 to 15 years.
Source: International Business Times
