An increase in deadly bird flu cases in China has health officials alerted as its spread to other countries is usually unnoticeable, avian flu being easily able to become a pandemic.
A recent CDC report has documented the risk of the disease evolving as it passes from one host to the other, leading the organization to investigate a vaccine to combat the new virus.

On a similar note, France has decided to slaughter about 600,000 ducks to curb the risk of an outbreak of bird flu. This adds up to a previous decision of the same kind which saw the birds of 300 French farms slaughtered. According to French Agriculture Minister Stephane Le Foll, the flu had spread much faster than it was anticipated.
Luckily, the virus does not spread easily from person to person, although it can be deadly to humans and other mammals that become infected. A previous strain of bird flu, H5N1, killed 60 percent of its infected hosts. The current strain is named A(H7N9).
A deadly disease pandemic is on the rise
According to the CDC, epidemics of avian influenza A(H7N9) have resulted in over 1,000 infections in China as they have been reported to the World Health Organization (WHO). The infected patients developed pneumonia and had to be interned in an intensive care unit. 44 percent of the reported cases ended up being lethal.
Because the disease is so dangerous, health organizations are looking for a vaccine, based on previous candidates developed back in 2013. Five epidemics occurred in Eastern Asia between 2013 and 2016, but the risk factor for human infections appears to be the same between all of them.
Apparently, the disease can be associated with exposure to birds, which is common in popular Asian markets. Samples were collected from people that frequented live poultry markets, and it was discovered that A(H7N9) was able to have two different reproductive sequences or lineages. More tests revealed that over 90 percent of the viruses surveyed had developed in the Yangtze River Delta.
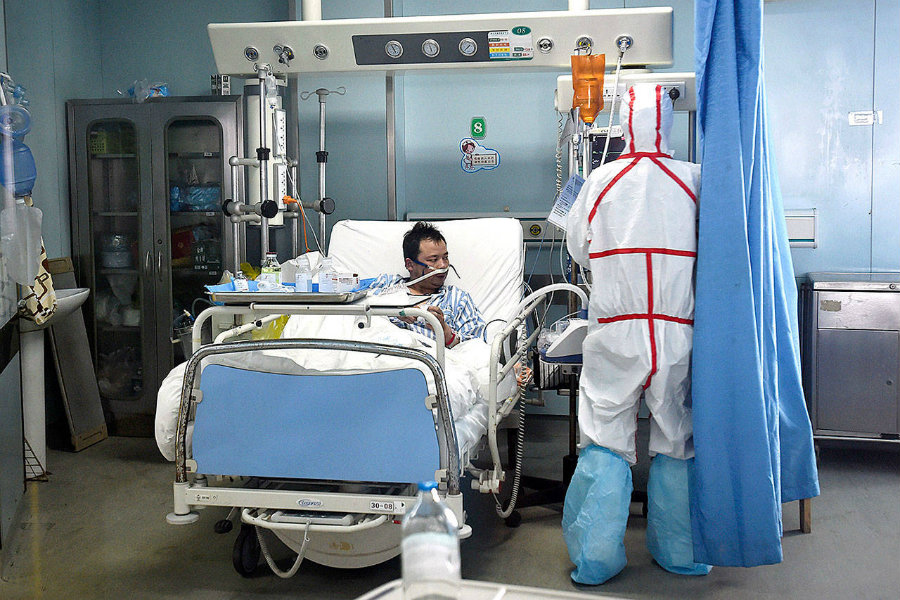
When the epidemic first started, the CDC has made use of the Influenza Risk Assessment tool to measure the risk posed by influenza A viruses. Currently, the risk for humans of contracting A(H7N9) remains particularly low, although it is quickly increasing its probability of becoming moderate to high-risk potential pandemic. To analyze this, WHO’s Global Influenza Surveillance and Response System experts met in Geneva last Wednesday to review the data that could categorize A(H7N9) as a pandemic threat.
Experts recommended developing at least two additional A(H7N9) vaccines to tackle the identified strains. This led the CDC to prepare a vaccine for one of the lineages, and the agency states that it will inform on how the vaccine could affect the risk assessment for the new strains of avian flu.
The CDC reports that influenza A viruses are of particular interest to public health, as it is classified by the Influenza Risk Assessment Tool to have “the greatest potential to cause a pandemic, as well as potentially posing the greatest risk to severely impact public health.”
It seems likely that infections with the virus associated with exposure to birds will keep occurring in China, and with that, the spread of the virus to neighboring countries. The CDC also deems possible that the human cases associated with the virus may pass undetected thanks to travelers returning to the U.S. after they visited an infected country.
CDC’s recommendations to prevent transmission
The first step is to minimize potential exposures by implementing policies that tackle the patient’s presence. The CDC recommends screening and testing patients that display symptoms, providing them with a facemask, and to have special care when dealing with patients that have just left an isolated airborne facility, which often serves as an incubator for new diseases.
For healthcare settings, it is recommended to place physical barriers to separate infected patients from the rest. It is also advised to oversee closed airway suction systems, for example, patient intubation, to reduce exposure related to medical procedures.
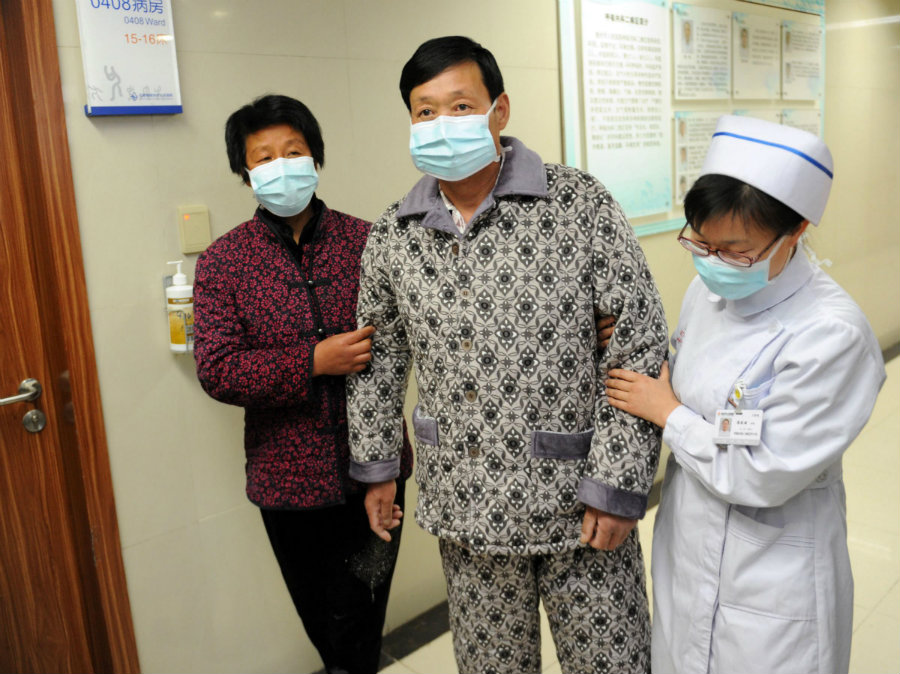
Health care providers who report respiratory symptoms after a documented and unprotected exposure to an infected patient should refrain from going to work. They should notify their supervisor and investigate respiratory hygiene while seeking out medical evaluation until they are officially no longer deemed infectious.
If unprotected exposure occurs, a ten day incubation test period is advised to monitor respiratory symptoms. In this case, the health care provider can continue working if a face mask is worn at all times during the incubation period while receiving antiviral medication.
Furthermore, the CDC calls for workplaces to educate their personnel on the disease, its prevention, and on how it spreads. Workplaces should implement stricter hand hygiene procedures, and health care providers are advised to wear gloves whenever they are entering an infected patient’s room or care area.
Source: CDC
